Face Masks: The Fake Science That Will Not Die
The Faucists STILL Argue Face Masks Matter
One would think that, with the passing of the COVID-19 Public Health Emergency, people would once and for all let the junk science and virtue signalling of face masks go once and for all.
The WHO Director-General concurs with the advice offered by the Committee regarding the ongoing COVID-19 pandemic. He determines that COVID-19 is now an established and ongoing health issue which no longer constitutes a public health emergency of international concern (PHEIC).
And one would be wrong. Face masks remain a grim tribute to the staying power of nonsense, even in the face of reality and research, as fans of the Giro d’Italia bicycle race recently found out.
Giro d'Italia followers coming into contact with riders will be required to wear masks in the wake of COVID-19 cases that hit the race and forced overall leader Remco Evenepoel to abandon the 'Corsa Rosa', race director Mauro Vegni said on Monday.
That’s right, even though COVID-19 has ceased to be a serious health issue anywhere in the world (including Italy), the merest hint of a case of COVID is enough for race officials to send fans scurrying to grab their face diapers once more.
When I say that COVID is not a serious health issue in Italy, I mean exactly that.
New cases in Italy are at an all-time low and have been almost since the start of the year.
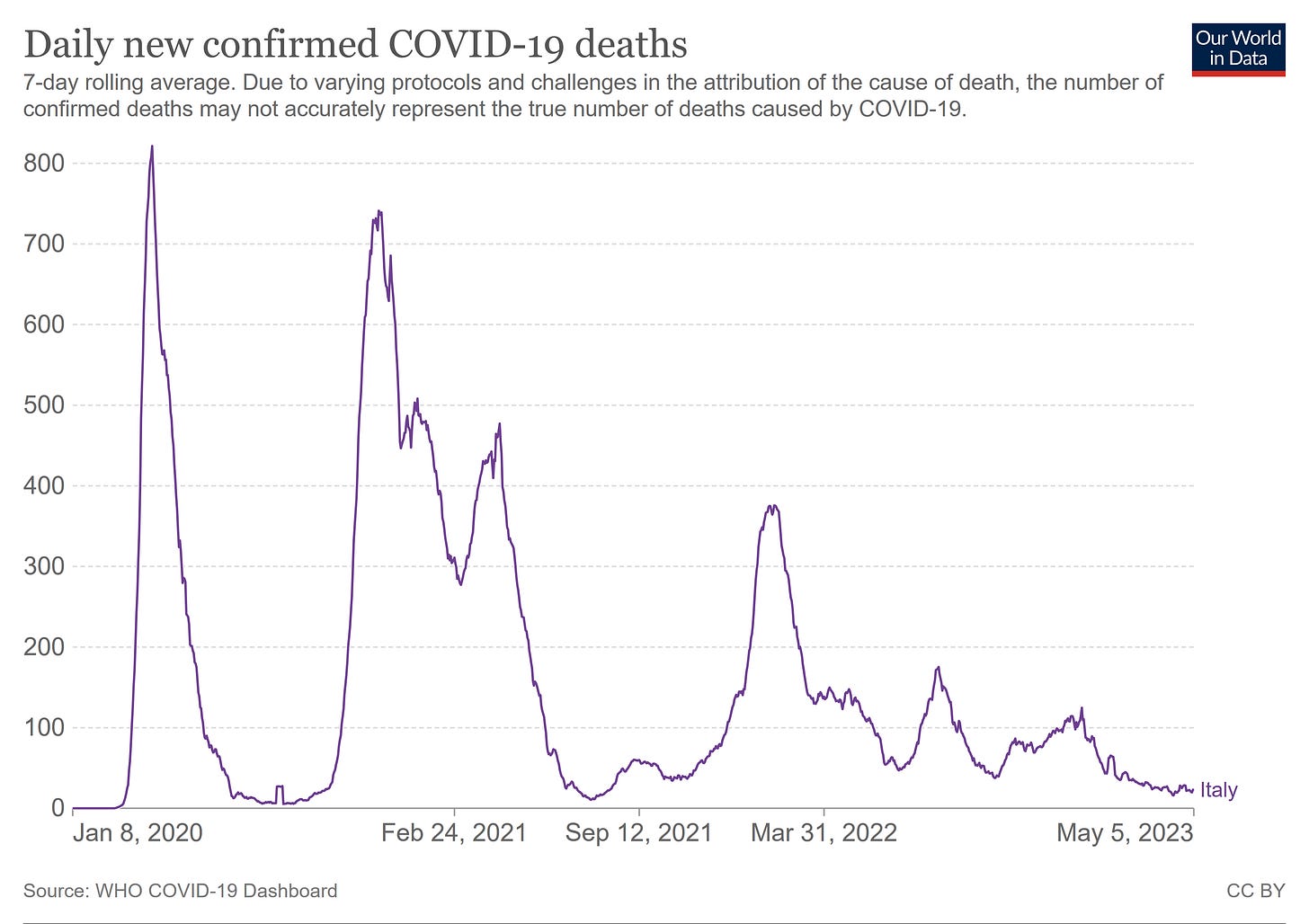
Confirmed deaths are also at an all-time low for the country.
COVID Hospital patients are similarly trending into nothingness.
COVID is simply not a burden on the public health in Italy at this time, and has not been so for months.
Yet despite this fading away of cases and patients, Italians are still fearful over the virus, so much so that merely testing positive for the virus compelled the race leader, Remco Evenepoel, to withdraw—even though the race rules did not require that.
Teams are not required to test their riders for COVID-19 and even in the eventuality of a positive case, they are not obliged to pull the rider out of the race.
Why did Evenepoel pull out? Because reasons.
Similar logic extends to the reaction race officials have had towards fans of the race, who must once more mask up if they are going to come out to watch the various race stages. Despite the endless array of peer-reviewed studies which show beyond any doubt that universal masking does not impede the spread of infectious respiratory disease, Italians are still virtue-signaling their intent to “fight” the spread of COVID.
Nor is this junk science fixation limited to Italy. Corporate media here in the United States continues to push the much disproven claim that face masks make a difference in COVID-19 spread, or of the spread of any infectious respiratory pathogen.
Even after the expiration of the US public health emergency declaration and with many Americans moving away from pandemic precautions, masks continue to offer some protection, reducing your risk of catching Covid-19 in a community setting like in a close doctor and patient interaction, according to the study, which reviewed the latest science on the protective quality of masks.
Because corporate media continues to push this arrant nonsense (and theories which have been repeatedly disproven can only be considered arrant nonsense and never anything else), we must yet again beat the dead horse of the number of studies that have shown literally for nearly two decades that universal masking does not affect the spread of infectious respiratory disease.
This was the state of the scientific understanding about the impact of masks upon the public’s health when mask mandates were first trundled out in April of 2020.
There are at least four separate studies on the effect of healthy people wearing masks as well as hand hygiene around symptomatic individuals:
There is the 2008 Hong Kong study of 198 households, which found "The laboratory-based or clinical secondary attack ratios did not significantly differ across the intervention arms." In other words, the masks made no difference.
There is the 2009 Australian study of 286 individuals across 143 households which concluded that "...household use of face masks is associated with low adherence and is ineffective for controlling seasonal respiratory disease."
There is the 2009 Hong Kong study of 259 households which found that among the mask-wearing groups "the differences compared with the control group were not significant."
There is the 2012 German study of 84 households comparing mask-only (M) and mask-plus-hand-hygiene (MH) strategies which found "there was no statistically significant effect of the M and MH interventions on secondary infections."
One point must be emphasized: these studies evaluate wearing masks as a mitigation/containment strategy. These studies do not offer any insight or commentary on the efficacy of an individual mask at blocking individual virion particles from entering the nose and mouth.
We must recall yet again that even the much-maligned World Health Organization, acknowledged that universal masking was ineffective at inhibiting the spread of infectious respiratory pathogens, and that the corporate media dutifully reiterated this stance.
Even as late as March 30, the World Health Organization (WHO) advised against wearing masks.
"There is no specific evidence to suggest that the wearing of masks by the mass population has any potential benefit. In fact, there's some evidence to suggest the opposite in the misuse of wearing a mask properly or fitting it properly," WHO executive director of health emergencies Mike Ryan said Monday.
The legacy media had been advocating the "no mask" position quite strongly even before March.
Even if there are cases next door, the answer is no, you do NOT need to get or wear any face masks—surgical masks, "N95 masks," respirator masks, or anything else—to protect yourself against the coronavirus. Not only do you not need them, you shouldn’t wear them, according to infection prevention specialist Eli Perencevich, MD, a professor of medicine and epidemiology at the University of Iowa’s College of Medicine.
"The average healthy person does not need to have a mask, and they shouldn’t be wearing masks," Dr. Perencevich said. "There’s no evidence that wearing masks on healthy people will protect them. They wear them incorrectly, and they can increase the risk of infection because they’re touching their face more often."
The message was clear: masks were bad. Do not wear masks.
This was the understanding the “scientific establishment” had regarding face masks in early 2020, and this was the understanding that was communicated to people in general regarding face masks in early 2020.
Nor has the actual science shifted or provided any new evidence to rebut this prior understanding.
While my early readings in 2020 had uncovered four peer-reviewed studies detailing how universal masking is ineffective against infectious respiratory disease, by last summer, that number had grown to at least fourteen—and fifteen if one includes a correct view of the data developed in the (in)famous Bangladeshi study.
In August of last year, statistician Jeffrey H. Anderson dug a little deeper and found a total of 14 Random Controlled Trials which failed to produce reliable evidence of any benefit from universal mask mandates as a public health strategy.
Even the large Bangladeshi study which the CDC claimed showed positive impact fails to deliver on that claim when one looks closely at the data—which is what Denis Rancourt, researcher with the Ontario Civil Liberties Union in Canada did, and found the study “fatally flawed.”
The cluster-randomized trial study of Abaluck et al. (2021) is fatally flawed, and therefore of no value for informing public health policy, for two main reasons:
The antibody detection was performed using a single commercial FDA emergency-use-authorized (EUA) serology test that is not suitable for the intended application to SARS-CoV-2 in Bangladesh (not calibrated or validated for populations in Bangladesh; undetermined cross-reactivity against broad-array IgM antibodies, malaria, influenza, etc.).
The participants (individual level, family level, village level) in the control and treatment arms were systematically handled in palpably different ways that are linked to factors established to be strongly associated to infection and severity with viral respiratory diseases, in particular, and to individual health in general.
Once one looks at the entire data set, as statistician William Briggs also did, the demonstrated efficacy of face masks in that study was 0.0026%.
Which means there are at least fifteen Random Controlled Trials which show “limited to no impact” for universal masking strategies.
Face mask mandates do not work against infectious respiratory disease.
The overwhelming position established by scientific data and research is clear and unambiguous: universal masking has no impact on the spread of infectious respiratory disease.
Yet despite this wealth of scientific data developed in peer-reviewed research, despite the existence of fifteen Random Controlled Trials—the “gold standard” of medical research—Faucist pseudoscientists continue to press a narrative that ignores this data, and even dares to falsely claim that it does not exist (emphasis mine)1.
Masking in the community has been a controversial mitigation strategy during the pandemic, in part because of the dearth of high-quality evidence documenting efficacy and in part because mask wearing has become politicized. Most published studies addressing mask efficacy have methodological flaws, and adherence to mask wearing has been suboptimal in virtually all. Demonstrating that masks work is difficult when they are not worn consistently. Although gold-standard evidence is not available, we argue that, despite the lack of clinical efficacy trials (as with the widely accepted practice of hand hygiene), masking in interactions between patients and health care personnel should continue to receive serious consideration as a patient safety measure.
Keep in mind that medical research has long identified the Random Controlled Trial as the “gold standard” in research2.
Randomized controlled trials (RCT) are prospective studies that measure the effectiveness of a new intervention or treatment. Although no study is likely on its own to prove causality, randomization reduces bias and provides a rigorous tool to examine cause-effect relationships between an intervention and outcome. This is because the act of randomization balances participant characteristics (both observed and unobserved) between the groups allowing attribution of any differences in outcome to the study intervention. This is not possible with any other study design.
Drs. Palmore and Henderson are apparently unaware of the fourteen exemplars of the “gold standard” available on this topic, sweeping away all such research with an unsupported statement dismissing the research as having “methodological flaws”, without ever stating what those flaws are.
Even worse, however, is the awkward reality that some the research they do cite actually contradicts their own thesis. The Klompas case study3 from 2021 documents three instances where face masks and PPE failed to prevent transmission of the SARS-CoV-2 virus.
We describe 3 instances of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) transmission despite medical masks and eye protection, including transmission despite the source person being masked, transmission despite the exposed person being masked, and transmission despite both parties being masked. Whole genome sequencing confirmed perfect homology between source and exposed persons’ viruses in all cases.
Research which challenges the efficacy of universal masking is an odd citation to use in defence of universal masking.
The final damnation to Drs. Palmore and Henderson, however, comes from the fact that their entire paper is at its core a straw man argument. Both of the main studies they cite to support their advocacy for masking focus on the mechanistic qualities of face masks.
The first study, from 2020, examines apparent modalities of virus shedding4. THis study also challenges their thesis, by acknowledging that surgical masks are inadequate to block aerosols.
Our findings indicate that surgical masks can efficaciously reduce the emission of influenza virus particles into the environment in respiratory droplets, but not in aerosols.
This is an important admission, as the next study they cite acknowledges that the SARS-CoV-2 virus does propagate via aerosols5.
SARS-CoV-2 is evolving toward more efficient aerosol generation and loose-fitting masks provide significant but only modest source control. Therefore, until vaccination rates are very high, continued layered controls and tight-fitting masks and respirators will be necessary.
The stated conclusions of their own cited studies argue against the face masks they advocate having any significant impact on the spread of SARS-CoV-2 virus, or of any infectious respiratory pathogen.
What these studies do establish, albeit unintentionally, is the importance of citing evidence and data relevant to the question at hand. No one has ever disputed the capacity of a face mask to inhibit the propagation of large respiratory droplets—that is the clear mechanistic function of a face mask. However, blocking droplets is not the same as preventing the spread of COVID, and as their own data establishes, face masks are not an effective impediment to the spread of COVID.
Whether the failure is due to the SARS-CoV-2 virus’ capacity to aerosolize, the difficulties in maintaining compliance with masking protocols over extended periods of time, or for some other aspect of infection and contamination not explored by these studies, the final analysis is that masks are ineffective against the spread of infectious respiratory disease. Their capacity to block large respiratory droplets, while true, is irrelevant.
Despite the very best efforts of the Faucists to argue otherwise, the extant data and evidence do not support universal masking as an impactful public health strategy. Even within the clinical setting, the extant data and evidence shows masking to be problematic at best, and far from an effective means of preventing the spread of COVID.
One point especially deserves emphasis here: opinions are not facts, and even expert opinions are at best a weak form of evidence, and arguably are not evidence at all.
Ironically, this statement is not my opinion, but is a position established by research and published in the scientific literature. A 2017 meta-analysis of clinical practice guidelines6 concluded that expert opinion ranked at the bottom of the pyramid of scientific evidence, and should be accorded only low validity if that.
Several depictions of the evidence pyramid consider EO as a level of evidence and place it at the bottom of the pyramid as a unique category, or combined with preclinical studies and case reports, implying low validity.
That meta-analysis does conclude that expert opinion, to the extent that it summarizes a compendium of evidence, may stand as a form of indirect evidence, and thus is more than just mere opinion. Outside of that aspect, however, expert opinion is still just opinion, and still just as minimally useful as evidence.
Despite the very best efforts of the Faucists to establish otherwise, opinion and authority are not evidence, and are never going to be evidence. Scientific scrutiny—actual scientific inquiry, not the pseudoscientific and ideologically driven narratives of “The Science™”—will always be driven by facts, data, and evidence.
It does not matter what this researcher or that researcher holds as a belief about anything, not about COVID, not about viruses, not about face masks, not about the nature of reality in general. It does not matter what I believe, or what you believe. Belief, when it comes to the appraisal of knowledge, is irrelevant. What matters are the facts, the data, and the evidence. All that matters is the facts, the data, and the evidence.
Now that health authoritarians world wide have decided to call time on the COVID non-pandemic, perhaps some of the lingering hysteria will die down surrounding the virus, and people will once again choose to follow the data, and not the frequently ill-informed “experts” and health authoritarians.
On face masks, the data is clear. On face masks, the research is in, and the evidence has spoken. Face masks are an ineffective public health strategy on preventing infectious respiratory disease.
Palmore, MD, T. N., and D. K. Henderson, MD. “For Patient Safety, It Is Not Time to Take Off Masks in Health Care Settings.” Annals Of Internal Medicine, vol. 176, no. 5, 2023, https://doi.org/10.7326/M23-1190.
Hariton, Eduardo, and Joseph J Locascio. “Randomised controlled trials - the gold standard for effectiveness research: Study design: randomised controlled trials.” BJOG : an international journal of obstetrics and gynaecology vol. 125,13 (2018): 1716. doi:10.1111/1471-0528.15199
Klompas, M., et al. “Transmission of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) From Asymptomatic and Presymptomatic Individuals in Healthcare Settings Despite Medical Masks and Eye Protection.” Clinical Infectious Diseases, vol. 73, no. 9, 2021, pp. 1693–95.
Leung, Nancy H L et al. “Respiratory virus shedding in exhaled breath and efficacy of face masks.” Nature medicine vol. 26,5 (2020): 676-680. doi:10.1038/s41591-020-0843-2
Adenaiye, Oluwasanmi O et al. “Infectious Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) in Exhaled Aerosols and Efficacy of Masks During Early Mild Infection.” Clinical infectious diseases : an official publication of the Infectious Diseases Society of America vol. 75,1 (2022): e241-e248. doi:10.1093/cid/ciab797
Ponce, O. J., et al. “What Does Expert Opinion in Guidelines Mean? A Meta-Epidemiological Study.” BMJ Evidence-Based Medicine, vol. 22, no. 5, 2017, pp. 164–69. http://dx.doi.org/10.1136/ebmed-2017-110798







Whenever I see someone wearing a mask, I shake my head and roll my eyes. They’re all just sheep who worship at the altar of Lord Fauci and the Holy Government.
Good article once again, Peter. What always amazed me was the people who were driving in their own car by themselves wearing a mask, Still see some of that!!!!!
Makes you want to ask them what they are thinking. Guess that stems from my BA in Psych from back in the 70s days.
Linking as usual @https://nothingnewunderthesun2016.com/